For Immediate Release
Contact: Sue Goin
sue.goin@sapphire-com
317.402.8690
BOSTON, October 10, 2017 — The concept of including minimally disruptive technologies by NICO Corporation within a pilot neurosurgical Enhanced Recovery After Surgery (ERAS) protocol was released in a digital poster (#4156) this week at the Congress of Neurological Surgeons (CNS) annual meeting. The observations support the ERAS precept of “minimal access surgery” (MAS) as an important component in reducing post-operative pain and complications, hospital length of stay, and costs.
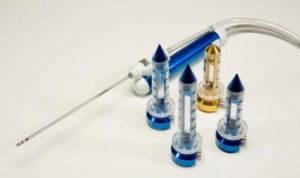
ERAS protocols improve patient outcomes by reducing surgical stress and maintaining homeostasis. Preliminary research suggests ERAS neurosurgery protocols that include minimal access surgery using minimally disruptive technologies like NICO BrainPath® and NICO Myriad® that are used in a trans-sulcal approach to brain surgery may have an influence on overall improved patient outcomes.
“ERAS evidence in other sub-specialties gives us an indication that neurosurgery specific protocols should be developed as part of the next generation of surgical care,” said Ronald Young, MD, neurosurgeon with the Brain and Spine Center of South Florida, Delray Medical Center, and poster co-author. Young has performed more than 100 surgeries using BrainPath and Myriad technologies, both part of the world’s first and only trans-sulcal system for standardized subcortical surgery known as the BrainPath Approach.
The poster – Inclusion of a Minimal Access Surgery Device System into a Pilot Neurosurgical Enhanced Recovery After Surgery (ERAS) Protocol – included 34 tumor cases with an age range of 23 days to 75 years and 13 vascular cases ranging in age from 48 to 64 years. Four detailed BrainPath patient cases exemplified improved outcomes, reduced length of stay, reduced operation times, and the ability to perform awake surgery. The poster is currently available online at the CNS and available online to the public following the CNS HERE. Access to the poster may also be obtained by emailing the CNS Press Room at marketing@cns.org.
According to Martina Cartwright, PhD, co-author and adjunct professor at the University of Arizona, performing minimal access surgery under “awake” conditions using short-acting anesthesia that promotes shorter operation times, as well as the management of post-operative pain, nausea and vomiting – all key components within the intra-operative and post-operative elements of the ERAS protocol.
“Many patients would likely benefit from a neurosurgery-specific ERAS program,” Cartwright said. “Essential components to consider in a multi-disciplinary neurosurgical ERAS protocol include pre-operative carbohydrate loading and minimally invasive surgical devices that facilitate ‘awake’ procedures, which improves overall patient satisfaction and reduces costs – all high priorities for hospital administrators as they work to optimize hospital efficiencies and improve patient experiences.”
BrainPath and Myriad work together as a system using imaging, navigation and intervention to achieve a true minimally invasive approach to neurosurgery using non-disruptive access, automated and non-thermal tissue removal and hemorrhage evacuation, and automated intraoperative tissue collection and preservation. Nearly 7,000 procedures have been successfully completed using BrainPath at more than 125 BrainPath Centers in Patented and FDA-cleared BrainPath and Myriad technologies by NICO Corporation used in minimal access trans-sulcal subcortical surgery.
the U.S., Canada, United Kingdom and Australia. BrainPath is patented and FDA-cleared for primary and secondary brain tumors, vascular abnormalities, and secondary bleeds.
The BrainPath Approach has three key components: 1) non-disruptive access to the subcortical space using BrainPath, 2) automated, non-thermal tissue removal with Myriad, and 3) intraoperative collection and preservation of tissue for post-procedural molecular evaluation and documentation of the anatomical location of each sample. During the final preservation step, tissue is treated like a discrete organ and immediately chilled. Standardization of these steps could lead to predictable and repeatable improved patient outcomes, as suggested in published clinical evidence.
Nearly 800 neurosurgeons, residents and fellows in the U.S. are trained on BrainPath. To learn more about BrainPath and other technologies used in the BrainPath Approach, visit NICOneuro.com, follow news updates on LinkedIn, and view surgical videos and patient stories on YouTube at NICOneuroCorp.